Cerebral Cavernomas
What is a Cavernoma?
Cavernoma are abnormal clusters of vessels with small bubbles (sometimes known as caverns) filled with blood that make them look like a raspberry or blackberry. Cavernomas are also known as cavernous angioma, cavernous haemangioma or cerebral cavernous malformation (CCM).
They can occur in the brain, brainstem, and spinal cord, but rarely in other areas of the body. Their size can range from microscopic up to several centimetres in diameter.
Cavernoma can enlarge but they are not cancerous and do not spread to other parts of the body.
There is little blood flow in cavernomas. Their walls, however, are weak which means there is a risk blood can leak within the cavernoma making it bigger and this can also leak into the brain outside it.
Diagram of a Cavernoma
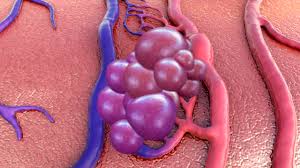
Incidence of cavernoma
Cavernoma occur in approximately 1 in 200 of the general population. Many are present at birth, but some develop later in life.
Some cavernoma are associated with other vascular malformations such as a venous anomaly.
Majority of people with cavernoma only have one lesion and no family history meaning they are sporadic and not usually inherited. A minority, however, (less than 50%) are thought to be the genetic type which means there may be a family history.
If you have more than one cavernoma or someone else in your family has been diagnosed with one as well as yourself, it is reasonable to suspect a genetic component. We know of three genes that can cause cavernomas. If this is the case, you may be offered or request genetic counselling to evaluate your family’s risk of cavernoma.
If you do decide to undergo genetic counselling and testing, there are some issues to consider: -
-Advantages: To know whether or not you have an inherited condition which means there is a potential for your relatives, siblings could have them. It also means there is a chance they can be passed onto your children and you can prepare for this.
-Disadvantages: If trying for a family or thinking of having children in the future, knowing your condition may be inherited can be both concerning and informative.
If it is confirmed that you have a genetic condition it may make it more difficult or expensive to get health or life insurance.
Ideally a clinical geneticist should council and support you in considering the factors and so help you make your decision.
If you are diagnosed with the inherited form (genetic type) of cavernoma each of your children has a 50 percent chance of inheriting the condition.
What are the Symptoms of Cavernoma?
Some people with cavernomas may have no symptoms and this is a completely incidental finding found when investigating or performing scans for another reason.
Unfortunately, one in three people with cavernomas eventually develop symptoms. These can occur at any age but most often between the ages 20 and 40.
In some people, cavernoma can cause haemorrhage or bleeding in the brain. In most cases the bleeding is small and may not cause symptoms but sometimes severe haemorrhages can lead to long term problems and may even be life threatening depending on the extent of the bleed and the position of the cavernoma.
Cavernoma are often diagnosed after a person has experienced symptoms including:
- A haemorrhage (may be small, but sometimes bigger leading to stroke like symptoms or a new or sudden severe headache)
- Seizures (most common first symptom in around 50% of people)
- Headaches
- Problems or changes in balance, speech, swallowing, vision, and tremors
- Stroke like symptoms
- Limb weakness, numbness, tiredness, memory, and concentration difficulties.
The type, frequency and severity of symptoms often depend on the location and size of the cavernoma.
Some locations of cavernoma are more dangerous than others in that they my cause more damage or problems if they bleed.
How is a Cavernoma diagnosed?
Magnetic Resonance Imaging (MRI) scans are the most reliable tool for diagnosing the presence of cavernoma.
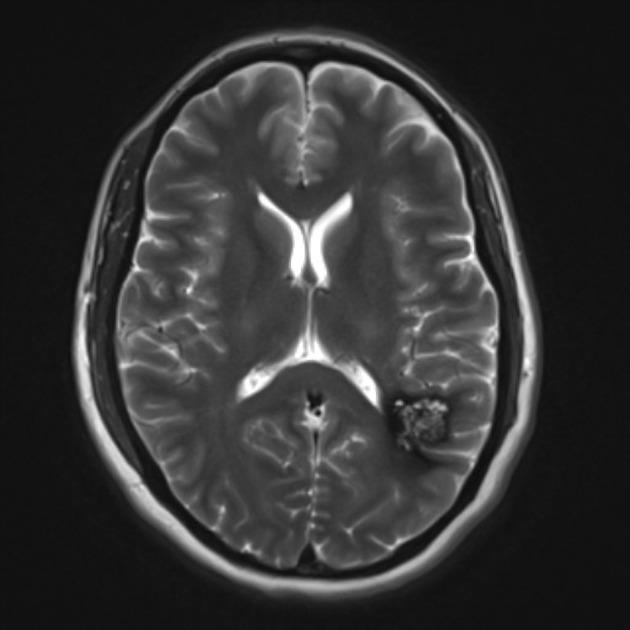
Other diagnostic tools include computerised tomography (CT) scans and angiography but often these scans cannot be relied upon and are often used to rule out other causes of symptoms.
Some cavernomas are diagnosed after investigation into other symptoms not definitively linked to cavernoma. As previously mentioned, these are known as ‘incidental’ cavernoma.
What causes brain cavernomas?
In most cases, there is no clear reason why cavernoma develop.
Less than 50% of cases are thought to be genetic.
There is a small links to previous radiation exposure; for example, some people have previously undergone radiotherapy to the brain.
Can a Cavernoma be prevented?
There is nothing you can do to prevent the development of a cavernoma.
How are Cavernomas managed?
Each person with a cavernoma is unique.
Symptoms of cavernoma can vary from person to person depending on size, location and the number of cavernomas.
A neurologist or a neurosurgeon can give specific medical advice.
- Conservative Management: (this is often recommended) ‘Watch and wait’ and observe changes, recent haemorrhage, or worsening symptoms. A ‘watch and wait’ approach may be recommended; this can include periodic MRI scans to monitor the cavernoma(s) after 12 months followed by annual appointments to check on changes to symptoms.
If this is your management then you should let us know if you develop new symptoms.
- Medication: Medicines may be given to help with symptoms for example, control of seizures and headaches. There is no known medication that can treat the cavernoma directly.
All cavernoma present a risk of bleeding. This is known as intracranial haemorrhage (ICH). Some bleeds occur and are not noticed whereas others cause symptoms. If a cavernoma has bled severely or a number of times causing symptoms then your neurosurgeon may offer surgical treatment to remove it. Some cavernoma, however, are in parts of the brain that make removal unfeasible because the risk of surgery is too high.
Treatment of Cavernoma
The decision to treat is made with your neurosurgeon who considers your wellbeing and personal wishes.
- Surgery: The most common reason for surgery is to reduce the risk and frequency of seizures or if you are having progressive symptoms of stroke.
Surgery is sometimes considered following a bleed. Some cavernoma bleed slowly enough that the body can reabsorb the blood and symptoms resolve with time. Others bleed more profusely and need urgent surgery to remove the blood and the cavernoma. Once a decision is made and discussed with you by your medical team; with your agreement you will be placed on the waiting list for treatment.
- ‘Stereotactic radiosurgery’ A less common treatment option. This includes a single concentrated dose of radiation therapy which zaps the cavernoma. Gamma Knife and CyberKnife are a non-invasive type of stereotactic radiosurgery. It is unknown how well either single or multiple cavernomas respond to this form of treatment.
- Genetic counselling may be available for some individuals and their families to determine if there is a genetic cause.
Everyday Activities
Having a cavernoma does not necessarily restrict your everyday activities. It will depend on how you are affected, whether you have had any treatment and what you feel you are able to do.
Lifestyle is important. You should not smoke and must keep blood pressure under control. You can keep your cardiovascular system healthy by regular exercise, keeping cholesterol under control and keeping alcohol within government guidelines.
If you have bled from your cavernoma you must give yourself time to recover and build up activity slowly as you are able. You must also take some time each day to rest. You should pace activities, keep well hydrated and keep a routine for meals and bed time
Information if you have bled from a cavernoma
You will need to pace yourself for the first month or more after going home because of tiredness or ongoing symptoms. If this is you, save your energy for the things you have to do and those you want to do. Looking after yourself in the early days of recovery is beneficial to your well-being in the long term. You may benefit from gentle exercise such as a short walk as well as a rest each day in the early days of your recovery.
Feelings of anger, frustration and sadness are not uncommon following a brain haemorrhage. This may be due to the condition but could just as well be due to the sudden life changing event and usually passes with time. If you are affected, you should talk to your GP as you may benefit from being referred to a psychologist to help you through this stage of recovery.
Enlist the support of your family and friends whilst you recover. They will be a great help with shopping, transport and support and will be the biggest influence in your successful recovery.
It is advised to have someone stay with you for the first week or so after going home.
Information if you have had seizures from the cavernoma
If you have had a seizure from the cavernoma you may need specialist management. A diagnosis of epilepsy is usually made by a specialist neurologist who will manage these symptoms, often through medication.
For your peace of mind and safety, you and your family need to be educated on how to manage the types of seizures you have and what to do if one occurs at home. Information is available for all patients who have epilepsy or have had seizures. This would be through your ward staff, the epilepsy nurse specialist team or the neurovascular nurse specialist team. The epilepsy nurses give a great deal of support including a dedicated phone line.
Living with a cavernoma
Symptoms caused by cavernoma are many and specific to the individual. You may find that many symptoms are made worse if you are tired, under stress or ill. This is particularly so if you experience seizures, headaches or have bled from the cavernoma.
Factor this into your recovery as you may need to look after yourself a bit more or ask for some help during these times.
Lifestyle is important when recovering. Lifestyle choices can make you feel worse or better.
Gentle exercise as you are able, eating well and preventing dehydration all help symptom control. Getting the right amount of sleep helps; too much or too little sleep can make you feel worse.
If you do too much, you may feel a little worse that evening or the next day. The general rule is if you want to do something and feel able to, then you can. If you find this makes you tired, then plan an easy day afterwards.
Memory problems: Memory problems can occur with cavernoma. If you have had a haemorrhage from it you may have problems with your short-term memory, attention and concentration. This usually improves but not always gets back to baseline.
Visual problems: Visual problems can occur because of the effects of certain cavernoma. Assessment and help can be gained if you have visual problems through an eye doctor called an ophthalmologist. If your vision has been affected, this may have driving implications. If you are registered partially sighted, you will be able to claim for free local travel.
Extreme tiredness: You will probably need rest once you get home particularly if you are having a lot of visitors or your house is very busy. Even simple tasks such as a walk to the local shop may leave you feeling exhausted. This will improve with time. You will know if you have done too much as you will be exhausted and may experience more headaches. This often happens early evening or the next day and means you have to take a rest! Pacing activities as well as regular exercise will help.
Headaches: Headaches are common and can persist with some cavernoma. If your headaches started after a bleed or treatment then they may ease with time.
Headaches can be triggered by dehydration, stress, illness, too much or too little sleep and missing meals.
Drinking 2 litres of water a day should help reduce the frequency and severity. Also, try and get back to a normal sleep pattern as soon as possible. Try putting some structure into your day, including meal times as this will help with headaches and recovery. Stopping smoking and reducing the amount of caffeine you take may help reduce the severity of headaches. Menthol sticks to rub on the forehead can help. Drinking a pint of water at the start of a headache may also help. If headaches persist and are troublesome you may need specialist management. This is particularly so if you are still taking regular pain medication after a few months.
Can I drive?
Driving restrictions are specific to the position of the cavernoma, the treatment, symptoms from it and whether it has bled or not. You have to inform the DVLA if you have surgery for a cavernoma.
If you have seizures you must not drive until you have been seizure free for 12 months. Other symptoms such as stroke like symptoms and changes to vision may affect your ability to drive.
You must speak to your medical team or neurovascular nurse to clarify driving restrictions. These decisions are made by the DVLA because driving involves many different cognitive and physical skills as well as multi-tasking, decision making and problem solving.
Driving regulations change all the time so please check with your doctor or nurse before going home from hospital.
Can I fly?
Yes. There are no particular restrictions on flying but you should speak with your doctor if you have any concerns or questions. It is advisable to tell your travel insurance company about your cavernoma.
Can I exercise?
Yes. You can exercise and we recommend you stay fit. We advise against extreme, excessive exercise that may push blood pressure up for a long period of time if your cavernoma has bled, is symptomatic and you should be careful if you have epileptic seizures.
Can I swim?
Yes. If you have epilepsy it would be advisable to swim with a companion, attend a swimming pool with a lifeguard present and inform them of your condition.
Can I have sex?
Yes. You can have sex when you are ready.
Can I drink alcohol?
We wouldn’t recommend alcohol if you have seizures or have recently bled from your cavernoma. Men and woman are advised not to drink more than 14 units of alcohol a week on a regular basis. You should spread your drinking over 3 or more days if you regularly drink as much as 14 units. Fourteen units is equivalent to 6 pints of average-strength beer or 10 small glasses of low-strength wine.
There is a risk of provoking a seizure if you drink too much. If you have seizures, excessive alcohol can lower the seizure threshold and make you more susceptible to them.
Can I smoke?
Smoking tobacco is not good for your health and it is advisable that you give up smoking completely. Smoking cessation clinics are linked to every G.P. Practice or you can ask for help during your stay in hospital. An advice number is printed at the end of this leaflet.
Can I take illegal drugs?
You should not take illegal drugs and amphetamines such as cocaine.
Can I try for a family?
If you have the genetic form of cavernoma and would like more information or support about genetic testing or genes associated with cavernoma you may want to get advice from you genetic counsellor before trying to conceive. Any decisions you make are personal and your genetic counsellor will be able to help with information and support.
Inheritance of Cavernoma Genes
If a gene change was found, genetics would be able to offer other members of your family. If they wanted a genetic test, they would need to ask their GP to refer them to their local genetic service to discuss the pros and cons of having the test.
Children are not normally tested for a cavernoma gene change unless the child had symptoms. Preference is usually to wait until the child is old enough to decide whether they want a gene test.
There is no specific management or treatment based in the genetic cause of cavernoma.
If a gene change is not found in someone with multiple cavernomas or a family history of cavernomas, it is likely there is still a genetic cause for the cavernoma. The gene change may not be found due to limitations of the testing method or there may be other yet undiscovered cavernoma genes.
Results take 4 to 5 months, and the geneticist would write to you once results received. If a gene change is found, you can let other family members know and they would be able to choose to have the genetic test if they wish and would require a referral from their GP to their local genetics centre.
Pregnancy and Childbirth
Studies so far show the risk of bleeding from a cavernoma does not change significantly during pregnancy. There is no increase in risk associated with vaginal delivery. The method of delivery should be based on general pregnancy and delivery considerations only.
If you have epilepsy or are concerned about seizures, it is important that your neurologist or epilepsy nurse specialist advises you early on in pregnancy, alongside the antenatal care provider. They will be able to advise you whether you should adjust the dose of anti-epileptic medication and provide guidance.
Self help
Cavernoma alliance UK offer practical advice and support for people who have cavernoma.
If you have any questions regarding any of the above topics or wish to discuss in further detail, please contact the neurovascular nurse team on 0151 556 3325. This is an answerphone, but we always contact you back if you leave a name and phone number
Walton Centre Contact Details
For any emergency see your G.P or go to your local
Accident and Emergency Department
Patient Experience Team provides a PALS service. 0151 556 3090
Neurovascular Nurse Specialists: 0151 556 3325
Or through hospital switch.
(Non-urgent enquiries – calls may not be answered the same day)
Walton Centre switchboard - 0151 525 3611
Dott Ward -0151 529 5633 / 5634
Cairns Ward - 0151 529 5637 / 5638
Caton Ward -0151 529 5628 / 5629
Sherrington Ward - 0151 529 5641 / 5642
Chavasse ward - 0151 529 5079
Lipton Ward - 0151 529 8884 / 8738
High dependency - 0151 529 5489
Intensive Care - 0151 529 5772/ 5773
For information regarding appointments or DVLA contact your
Consultant’s secretary.
Useful Contact details
NHS 111: 111
Telephone advice if you need urgent medical help fast but it is not a 999 emergency (or you do not have a GP)
Website: http://www.nhs.uk and search ‘emergency and urgent care’
D.V.L.A. Driver Vehicle Licensing Authority,
Drivers Medical Group, DVLA, Swansea, SA99 1DL.
Medical Enquiries: 0800 032 5202
Access to work https://www.gov.uk/access-to-work
Cavernoma alliance: 01305 213876 www.cavernoma.org.uk
The Brain Charity: 0151 298 2999.
Offers practical help, emotional support and social activities for people with neurological injury. And their families/carers
Working Life Service at The Brain Charity: 0151 298 3288
Brain and Spine foundation: 0808 808 1000
NHS Free smoking helpline:
0300 123 1044 (England)
0800 085 2219 (Wales)
Advice on Alcohol: 020 7766 991
- Last Updated:01 September 2023
- Review Date:30 September 2027
- Author:Debbie Brown
- Summary:
Cavernoma are abnormal clusters of vessels with small bubbles (sometimes known as caverns) filled with blood that make them look like a raspberry or blackberry. Cavernomas are also known as cavernous angioma, cavernous haemangioma or cerebral cavernous malformation (CCM).