Anterior Cervical Discectomy
Information for patients undergoing an anterior cervical discectomy
Admission to hospital can be a daunting experience for most people. The following information is designed to give you information about your stay at The Walton Centre and what to expect. This information is intended as a guide and may vary depending upon your individual requirements for further information please see patient information on British Association of Spine Surgeons website (spinesurgeons.ac.uk/Booklets)
The Walton Centre is a regional unit that admits patients 24 hours a day depending upon the urgency of their condition. Although every effort is made to ensure your admission goes ahead as planned, occasionally it is necessary to cancel planned surgery at short notice.
What is a anterior cervical discectomy?
The surgical procedure that you are to be admitted for is called an ANTERIOR CERVICAL DISCECTOMY. This is performed for someone who has a prolapsed (slipped) disc in the neck area. This can be performed for 2 reasons 1. If you have a slipped disc in the neck trapping an individual nerve root or, 2. causing compression to the spinal cord itself.
The spine is composed of small bones called vertebrae which all sit on top of each other to form your spinal column. The neck area (cervical spine) is made to be very flexible so we can move our head and see around us, this flexibility increases the chance of wear and tear to this structure. There are 7 bones in the cervical spine, to stop these bones from rubbing on each other you have intervertebral discs. These are soft cushions of tissue which sit in between each of the bones in your spinal column and act as shock absorbers. The discs lose flexibility due to wear and tear, the tough fibrous outer layer of the disc can split and no longer hold the gel like substance in the centre. This can cause it to bulge out causing pressure to nerves or spinal cord resulting in your symptoms
A prolapsed disc occurs when one of these cushions (discs) slips out slightly and puts pressure on one of the nerves, or the spinal cord itself, causing your symptoms.
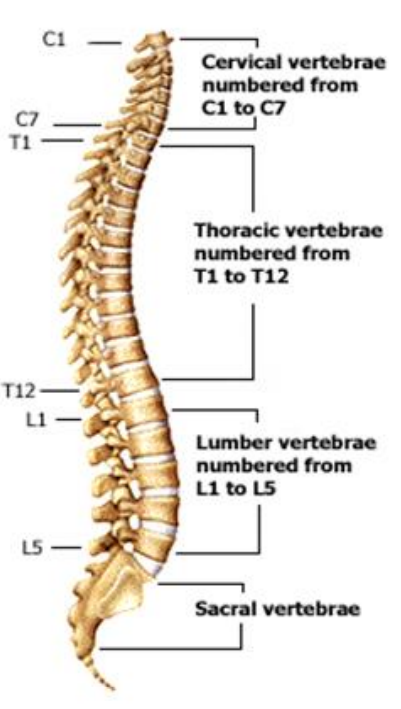
The spinal column forms a bony cylindrical tower, and down the centre of this runs the channel for your spinal cord. The bony spinal column protects the delicate spinal cord structure. The spinal cord acts in a similar way to a telephone exchange passing information from your brain to your body and back again. At the level of each bone (vertebra) your spinal cord sends out a nerve, one on the right side and one on the left side. These nerves contain millions of nerve fibres, to transmit messages to and from the body. They send messages to tell us about the sensations we are experiencing such as pain, temperature and the ability to know where our limbs are without looking. They also send messages that allow us to move our bodies.
The spinal cord and nerve roots are surrounded by a fluid called cerebrospinal fluid (CSF) and this is contained within a membrane, or covering, called the dura mater, rather like the thin layer that covers a boiled egg allowing this to protect all the structures.
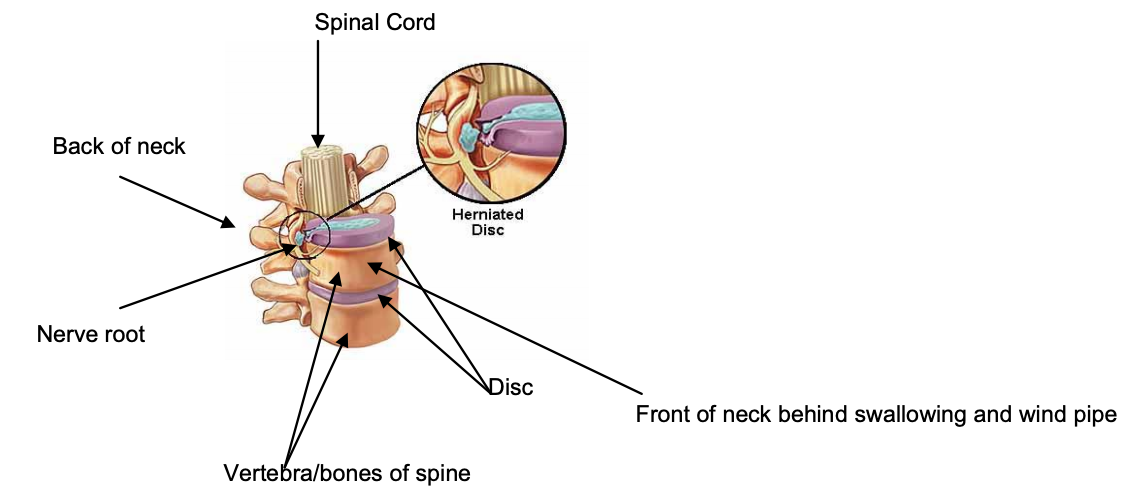
What does a prolapsed disc cause?
Prolapsed discs can cause various symptoms depending on which nerves they press upon. Prolapsed discs in the neck area, which cause pressure on an individual nerve on the right or the left side, mostly cause symptoms in the arms.
Usually, the pressure on the nerve causes pain to radiate down the arm in the path that the nerve travels from the spinal cord down the arm. Occasionally, there may be numbness or weakness in the arm or hand, possibly with some tingling or unusual sensations such as pins and needles.
Sometimes if the prolapsed disc causes pressure on the spinal cord itself, this can cause symptoms affecting the arms, hands, legs, bladder and bowel. This is known as cervical mylopathy and can also cause clumsy hands, difficulty with fine finger movement tasks, balance issues causing unsteadiness when walking.
Treatment
Most attacks of pain and altered sensation settle themselves after a few weeks and will not require any surgery. 6 out of 10 patients can get better within 6 weeks, 7 out of 10 patients feel better by 3 months.
The other options for treatment are:-
• Allow your body to heal naturally and the symptoms will resolve as the slipped part of the disc reduces by itself, and the pressure on the nerves is relieved.
• Physiotherapy treatment, Pilates, Tai Chi and Yoga all of which will help with posture and muscle tone.
• Managing the pain with medication. In some cases osteopathic treatment or injection therapies may help.
If the pain does not settle spontaneously without any intervention and persists with a degree of severity then surgery can be considered. There is a balance to reach between allowing recovery without intervention, any continued deterioration and the risks of surgery.
Surgery allows considerable relief of pain in most cases. It has less effect on any sensory changes you may have, such as pins and needles and numbness. If there is some muscle wasting (loss of muscle bulk), then this is usually irreversible but this may possibly be improved by a little focused exercise after successful surgery. Surgery also allows the relief of symptoms earlier than of you wait for the natural healing process to complete.9 out of 10 people get good relief from their arm pain following surgery, but it does take time to settle. Some patients find they get a flare up of pain approximately 7 days post surgery, then this gradually starts to settle, and can fluctuate for many months, surgery usually does not give instant relief from arm pain. Although some people do find surgery helps their neck pain, the main aim of surgery is to improve the arm pain and is not aimed at neck pain.
In the case of patients with compression to the spinal cord, causing problems with hand dexterity, walking and bladder/bowel function (cervical mylopathy) the aim of surgery is to prevent deterioration rather than to gain improvement. Any improvement after surgery for spinal cord compression can take many months (12-18 months for maximum outcome) and may never improve, this is because any damage to the spinal cord, from the pressure of the disc, cannot be repaired. It is not possible to predict your recovery, you have to wait and see whilst engaging in any rehabilitation programme/physio etc.
What does surgery involve?
A discectomy allows the disc which is causing the pressure on the nerve or spinal cord to be removed with minimal disturbance of bone and tissue. This is achieved with microscopic surgical technique. Discectomy involves having a small horizontal incision just below the collar line of the neck, at the front while you are asleep under general anaesthetic. A microscope is used for the surgery to give a better picture of the tissues and to minimise the disturbance to the surrounding structures, improving the accuracy. The front of the spine is exposed, the disc is approached from the side and the disc that is pressing on the nerve is removed. At this time they can also remove any bone spurs (overgrowth of bone) causing pressure to nerves that have occurred as a result of degenerative change in the neck.
Once the disc is removed, the Surgeon then inserts a small cage, which looks like a polo mint in shape and size, into the space left from where the disc was taken. A cage is made of titanium metal, reinforced plastic or carbon fibre and is used as an aid to stabilising the structure. A cage is a small permanent implant in your spine, which goes between the vertebra where the disc has been removed, it supports a bone graft whilst it heals and is not removed.
A graft is used for bone fusion, this is an addition of either your bone or donor bone (bone from someone else), into the operation site to stabilise the bones of the spine. When the disc is removed the new cage has bone placed in and around it to allow both the bones above and below the cage to fuse together into one section.
Fusion is also sometimes needed because bone is removed during surgery to allow access to the disc space or if your bones normally have too much movement in them, this can make them unstable.
They then, sometimes need to be packed with bone in order to keep the structure stable and allow fusion of the spinal bones (the spine to become solid and stable) following surgery. Fusion takes 3-6 months to occur.
The bone used to pack the space is either your own taken from part of the spinal column around the site of your surgery, artificial bone, or donor bone that is accessed from a source that has undergone rigorous testing. DBM (demineralised bone matrix) is a product made of bone fibres that have been shown to provide scaffolding for your own bone to build upon. Very occasionally bone may be taken for fusion from the front part of your pelvis, just behind your hip (during the operation) but this is only used rarely.
In some patients a metal (titanium plate) is applied to the front of the spinal bones to add stability. The plate is placed over the front of the spine and screwed into the spinal bones above and below the disc space that has been fitted with the cage.
What are the advantages and disadvantages of surgery?
The following information is to help you understand what we are offering you and why. Please remember, agreeing to surgery is your decision. The job of our team is to present you with the facts and options as we see them. You have the right to change your mind at any point in time, if you wish for further explanation at any time please just ask one of the staff.
The advantage of surgery is that it can give significant chance of relief from pain. However there is no guarantee that there will be any improvement in any weakness or numbness that you have had prior to surgery.
The Risks
This operation is a very common operation performed at The Walton Centre, but as am sure you are aware it does not come without any risks. All the risks will be discussed with you prior to your surgery and although they are not common you should be aware that there is the potential for them to occur.
1. Risks from anaesthesia (being put asleep for your surgery), please read you anaesthetic booklet
2. Risk of Deep vein thrombosis (DVT, blood clot in your leg) or Pulmonary embolus (PE, blood clot in the lung),The risk is rare and we use special surgical stockings, and blood thinning injections where appropriate to reduce the risk.
3. Risks from positioning during surgery and equipment used, this can include skin injuries, eye complications, most severely blindness but this is exceptionally rare. Special gel pads/protection are used during surgery to minimise the risk of these complications. Diathermy pads are used which is an adhesive pad placed on the skin, usually the thigh area, to minimalise heat build up, this can cause skin irritation and in exceptional and very rare cases a skin burn
4. Small risk of persistent or increased pain.
5. Risk of injury to the nerves or spinal cord causing weakness or numbness this occurs in less that 1 out of 100 patients, it is more common if this is a repeat operation when it increases to 10 out of 100 patients. In the extreme this can result in total paralysis (unable to move from the neck down) but this is an exceptionally rare complication.
6. Sore throat/swallowing problems due to manipulation of the throat structures during surgery to allow access to the front of the spine (this should settle down in a few days). This can very rarely be permanent.
7. Vocal cord problems, hoarse voice (although this should settle down within a few days). This can very rarely be permanent.
8. In theory there could be injury to the nerve for sweating, eye lid and the pupil (Horners Syndrome) although this is also exceptionally rare (1 in 100 patients).
9. Leak of spinal fluid, this is where there is a tear in the lining which surrounds the nerve roots, this occurs in less than 1 in 100 patients. This is repaired with stitches, a patch or special glue. The worst case scenario is that further surgery is required to repair the leak but this is extremely rare (0.05%)
10. Infection, superficial wound infections can occur in approx. 4 out of 100 patients and are easily treated with antibiotics. Deep wound infections occur in less than 1 out of 100 patients, but these can require further surgery and long courses of antibiotics. Infection risk includes infection from the MRSA bacteria (infection with MRSA is very rare). Any infection can result in Sepsis but again this is exceptionally rare. Those with weakened immune systems, diabetes or taking steroid medication are more at risk of infections from surgery.
11. Bleeding or haematoma (collection of blood), in very rare circumstances this can require a further operation as this can cause pressure on the windpipe, resulting in difficulty breathing or swallowing. Damage to major blood vessels around the spine can cause death but the risk of this is rare (1 in 10,000 cases)
12. Wound drain problems, requiring removal in theatre, whilst under anaesthetic, which again is very rare.
13. In patients having a graft or cage there is potential for the graft or cage to slip forward and move out of the correct position (2 out of 100 patients). There is also possibility that the bone does not fuse which can affect 5 out of 100 patients.
14. The level of surgical intervention, not fusing causing pain which may need further surgical intervention, again this is exceptionally rare.
15. Problems at the levels above or below the surgery, due to the level either side of the disc removal being fused, this can sometimes put pressure on the level above or below the surgery, causing problems over time.
It is possible for a prolapsed (slipped) disc to occur at another level in the spinal column at some time in the future.
As already mentioned complications are rare, but we have a duty to inform you of all possible complications, even though lots of them are very rare. If you are worried about any of the aspects surgery you will have the opportunity to discuss any concerns prior to surgery and following your hospital admission.
Pre-operative assessment
It is important, if you have any changes in your pain or symptoms and also if you develop any new medical conditions or are unwell, you speak to spinal nurses or your consultant’s secretary at the earliest opportunity but definitely prior to attending for your admission.
In order to gain the information we need to ensure your safety during your surgery, once you have agreed to surgery you will be required to complete a pre-operative assessment online. You will be provided with the information you need on how to complete this. The information you provide will be reviewed by one of the pre op nurses. Once this is done you will be contacted to explain the next steps that will be applicable to you and the procedure you are undergoing.
Your admission will not be arranged until you have completed your pre-operative form as this is important in deciding if you need any additional assessments. It is essential we ensure your maximum safety for surgery. If you are having any problems completing the on line documentation then please inform the pre op nurses.
For some patients you will only need to attend for some blood to be taken for testing, and routine swabs. Some patients will need to be spoken to by phone to clarify medical details, some will need to come in to clinic to be seen and examined.
It is very important that you complete your pre-operative questionnaire with all the details as accurately as possible, as inaccurate information may delay your surgery
If you do have to attend for an assessment it may include:-
1. A member of the team will discuss your medical history (your past operations and any medical conditions you may be suffering from) with you and you will be examined.
2. You may be reviewed by an Anaesthetist; he/she will have a chat with you and discuss any relevant medical history and explain what having an anaesthetic will involve.
3. You will have some blood tests performed.
4. If any x-rays or a heart trace (ECG) are required these will also be done.
5. Your medication may be prescribed; it would be helpful if you could bring with you any medication that you are taking or a list of your medication and doses. It is very important that you tell us about all your medication, including all prescribed medication, medication you buy and any herbal remedies. It is especially important that you tell us about any medication that may thin your bloods.
An appointment will be organised for you and sent to you if you are required to attend for this.
Some patients may not have a pre-operative assessment of any type, this can be for many reasons, for example, you are admitted urgently or as an emergency and there is no time for all of this to be completed. This is not a problem, because everything you need will be done the day you are admitted. Your surgery in this situation is normally the following day. You will not go home overnight.
Please be patient whilst we complete all of our assessments. It is important that we ensure everything is completed to ensure your safety. Occasionally we need to postpone surgery if your pre-operative assessment indicates that there are more tests or assessments needed before we proceed with your surgery. We understand that this is frustrating, but we will not proceed until we have all the information we require to ensure your maximum safety.
Admission to Hospital
You will be able to eat and drink up to midnight the night before your surgery and drink clear water only up to 6am on the morning of your surgery. You will then be able to have sips of water only from 6am until you go for your operation. This will be clarified for you prior to your admission. Most patients will be admitted the day of their surgery at approx. 07.15 having followed the fasting instructions above.
It is advisable not to bring any valuables with you into Hospital as the Hospital does not accept any responsibility for their safety.
When you arrive you will be seen in an admission area and then informed which ward you will go to after your surgery.
The Day of Surgery
You will continue to be kept fasted (nothing to eat or drink) and need to wear a theatre gown, we would ask that you have a bath or shower the morning of your surgery before you leave home.
Your details will be checked with you on the ward before you go to theatre. You will be wearing a wrist band and have to answer a list of questions, for example, your name, date of birth and confirm that you have removed all jewellery, underwear and make up etc.
You will be collected for theatre and taken to the theatre reception area, where the Nurse will check you details again; whilst this can appear repetitive it is all done to ensure your safety. From there you will be taken to the anaesthetic room, where your details will be checked again. We have a robust safety check list which includes asking you to confirm what operation you are having, your symptoms, which side of the body and where you experience them, do not be concerned, this is for safety only and not because of any queries about your surgery. Once this is done the anaesthetist will give you your anaesthetic medication, and once you are asleep you will be taken into theatre and surgery performed.
The surgery will be performed by the consultant or one of his team. It is common for x-rays to be used in theatre to assist the surgeon with checking the correct position of the neck bones.
After surgery you will be taken on your bed into the recovery room where you will be monitored whilst you wake up from your anaesthetic, and you will be made comfortable for your transfer back to the ward. You will be transferred back to the ward after spending approximately 1-2 hours in recovery. On return to the ward you observations i.e. blood pressure and pulse, will be checked regularly, as will your wound and your limb power and movement.
An intravenous infusion (drip) will be in your hand until you are awake enough to eat and drink again. You will be able to have sips of water a few hours after you return to the ward and then increase this as you feel well enough.
You may require a wound drain, this is a small plastic tube located just beneath the skin that comes out of the skin near wound and is attached to a plastic collection device. It drains any excess fluid/blood away from the wound but is not always needed. This is usually held in place by a small stitch. This is usually easily removed by removing the stitch and gently pulling the tubing out from under the skin. It is usually removed the day after surgery. In exceptional circumstances this may need to be removed with a further operation but this is an exceptionally rare requirement
If your surgery is early in the day then you should be able to get out of bed and mobilise around the ward the evening of your surgery. Once you have recovered fully from the anaesthetic we will be happy for you to be out of bed.
It is normal to feel some discomfort in the wound area after surgery and around the back of your shoulders (due to positioning in theatre) but we will manage this with appropriate pain relief medication.
The Day after Surgery
The day following surgery your drip will be removed, your wound will be checked and if you have a wound drain, it will be removed. Taking the wound drain out requires the nurse to remove the stitch holding it in place and gradually sliding the drain tube out. It is not normally painful and they are usually easily removed. In very rare circumstances the drain may need to be removed in theatre however this exceptionally rare.
If you have not already been out of bed you will be expected to get out of bed and move around. You may be seen by a physiotherapist if needed, however a copy of the exercises are in the back of the book to aid your recovery.
You should be careful not to do excessive movements of your neck for the first week in order to protect the position of the cage/graft until it settles into place. Normal movement is expected.
Some patients will have an x-ray of their neck the day after surgery, some patients may need to wear a neck collar, this depends on the type of surgery performed. The medical staff will make this decision based on each individual patient.
One of the medical/specialist nursing team will check how you are managing. Following this you will normally be able to go home late morning or in the afternoon. It is quite normal practice to go home the day after your operation. Occasionally some patients who have had more extensive surgery may need some extra time in Hospital to recover. This is often just an extra day and is not usually more than a few extra days.
Pain medications
You may be taking 2 types of medications for pain, many patients come in for surgery having taken pain medication for a long time, such as Gabapentin, Pre gabalin, Amitriptyline, Duloxetine, or opiod based medication e.g morphine etc. Your doctor or specialist nurse may recommend, following your surgery, that you take a strong opioid medication alongside other painkillers such Paracetamol and your usual medication. This is to relieve the additional pain that your injuries, illness or surgery has caused.
When you are discharged, as well as your normal medication, you may be given strong opioid medication to take home. It is important that you do not exceed the maximum dose prescribed for you. It is also important that you do not take any other painkillers that have not been prescribed by the hospital at the time of your discharge. This may result in you having too much pain medicine and cause the risk of severe side effects.
If you were not already taking opioid medicines before admission to hospital, you should not need to take them for a long time. The additional pain medication, prescribed whilst you are in hospital, is only intended to be short term. As you recover and your pain reduces you will be able to slowly reduce taking the medicines.
Any medication you were taking prior to surgery should not be stopped suddenly and once you have recovered from surgery, after a few weeks, as you pain settles, discuss with your GP a reducing regime for your medication You should ask you GP to review your medicines to ensure you are not taking them longer than necessary and also to ensure they are reduced safely as abrupt stopping of some medications can produce side effects.
Discharge Home
Getting home – Please arrange for a relative or friend to collect you. You will not be able to drive or use public transport. You can go home by taxi if a member of your family or friend can accompany you. If you cannot get transport arranged then we can arrange hospital transport, however travelling with a relative or friend would preferable if you can organise this.
Medication - Medication can be organised for you to take home, if required. Unfortunately, if we arrange medication from our pharmacy then this can mean you need to wait until later on your discharge day for it to arrive.
Sutures - Some patients will have dissolvable stitches in place, some will have stitches that need removal, and some may have metal clips. Your stitches/clips will be due to be removed approximately 7 days after your surgery (in some cases longer, but this will be clarified with you before you go home). Most patients make an appointment to get this done by their GP, Practice Nurse or walk in centre. If you do not have access to this then a District Nurse can be organised to check your wound and remove your stitches (dissolvable stitches will only need to be trimmed at the ends) If needed then the date of your District Nurse visit will be given to you before you leave the ward. Please make sure that if you are not going home to your usual address and you are going to stay with someone else you inform the staff to ensure that the District Nurse comes to the correct address.
Wound Care - Should you have any problems with your wound after your surgery, even if your GP or District Nurse are managing this, it is very important that we are also informed as we may need to monitor your more closely. We would like you to contact us if there is any redness round the wound, wound leakage, or you have a temperature.
Please phone either:-
Spinal Nurses on 0151 556 3424
Tissue Viability Team on 0151 556 3601
You can bath or shower, but please aim to keep the wound dressing dry, until it has healed and any sutures/clips have been removed.
Pain - It is not unusual for you to get increased pain or altered sensation for a few days to a few weeks after surgery as your spinal cord and/or nerves recover from your surgery. It is important that you stay mobile and continue with your physiotherapy exercises following discharge. Some patients will experience a flare up of arm pain of symptoms approx. 7 -10 days post surgery, this usually settles over time, but it is not unusual to get fluctuations in pain/symptoms over many weeks/months.
Activity - Remember that you have had an operation and it is usual to feel tired after this. Pace yourself and gradually build up your level of activity. Doing small things often, rather than all in one go is more sensible. You should progressively return to your normal daily routine as quickly as possible. You can undertake all the usual activities of daily life as you feel comfortable this includes walking, shopping, driving and sexual activity
Research has shown that patients who return to normal routine as quickly as possible make the best recovery. You should progressively return to your normal daily routine as you continue to recover. You can return to work as soon as you feel you can cope even if you feel uncomfortable. Heavy lifting should only be performed in the correct way and should be avoided for the first three months.
Surgical stockings - You should wear your surgical stockings for up to 6 weeks post-surgery, if your mobility is restricted or 2 weeks if you are fully mobile to reduce the risk of DVT (blood clots in the legs), and we advise not to fly for 6 weeks post surgery, again due to the risk of DVT
Driving - You can drive when you can have a full range of movement and you must have full movement to allow you to have full control of the car, this includes being able to do an emergency stop. This is usually a few weeks after surgery.
Work - You can return to work when you feel able and this can depend on what your job role involves. Those with desk based roles may feel comfortable to return to work 4-6 weeks post surgery, but would need to be able to get up and move around to prevent stiffening in the neck area. Those with more manual jobs may need to wait the full 3 months before being able to return. Please discuss this with your nurse specialist or medical team if you are unsure.
When will we see you - You will be sent an outpatient appointment for approximately 3 months following surgery by post to either come and see us, or for us to speak to you by phone, so we can check you are recovering well. Here you will be seen/spoken too by either a doctor or a nurse specialist.
Concerns - If you have any queries before then please do not hesitate to contact the spinal nurses on the advice line 0151 556 3424. Please leave you name and telephone number clearly on the answer machine so we can call you back. We try to answer the messages every working day. We work Mon- Fri 8am-6pm, we do not work weekends. We do spend a lot of time on the wards and in the out patient clinics seeing patients, so please be patient, we will call as soon as we can.
The physiotherapy section gives you advice on what you should be doing when you go home.
Physiotherapy Following Discectomy Surgery
Physiotherapy
This information is intended to answer the most commonly asked questions. Any further enquiries can be directed to the Physiotherapy department.
On your first day post operatively, it is perfectly safe to:
• Be up and walking around.
• Perform daily activities such as dressing and washing.
• Spend time sitting out in your bedside chair, regularly changing your position is advised.
General advice
It is safe to continue with all regular activities such as cooking, cleaning, shopping and sexual activity.
You can sleep in whatever position is easiest for you.
You may continue to have some neck/ arm discomfort or changes in sensation especially for the first 12 weeks, this is normal. Often this type of surgery is performed to ensure symptoms do not get any worse. Your medical team will have discussed this with you pre procedure.
There is no evidence to say that returning to activity and exercise leads to any adverse effects or the need for re-operation.
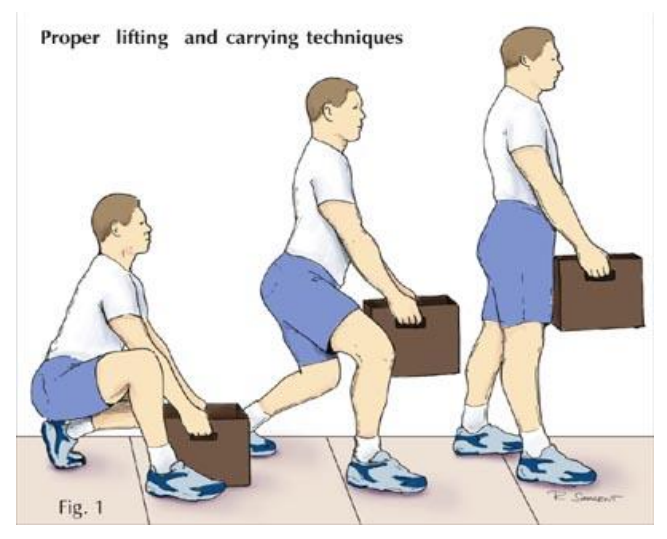
Lifting
There is no restriction in bending forwards to pick up light objects or putting on your shoes and socks. We think it is sensible to avoid heavy lifting where possible to begin with. You can resume lifting when you feel able to do so. There is no given weight limit that we advise because everyone has their own usual capabilities. You can gradually increase the amount you do until you are back to your typical day to day routine.
Driving
You can return to driving as soon as you can sit comfortably, perform an emergency stop and that you feel safe to do so. This is a self-certification, meaning you decide if you are safe.
Work
Returning to work and normal activities will help your recovery and you should aim to do this as soon as possible. People who return to work sooner have been shown to have better outcomes. You can return to work as soon as you feel you can cope, even if your back is still uncomfortable. You may wish to grade your return to work. It may take slightly longer to be able to return to a more ‘manually heavy’ job. It is normal to feel tired when returning to work after a period of sickness absence. You should plan to pace yourself and take regular breaks.
Exercise
General activity and exercise has been shown to be safe in this patient group and indeed is beneficial for your overall health.
We have included an exercise programme however general activities that you may already enjoy have been proven to be as effective therefore you should look to gradually resume these. For example; hiking, swimming, cycling, jogging, yoga and Pilates. Keeping a record/ diary may help you in guiding your progress. Some discomfort is normal when re-commencing activity; you should work within reasonable limits. Lower intensity exercise should be started first progressing to higher intensity over a period of weeks.
You can also safely return to recreational sports such as football, cycling or golf in a gradual manner. For specific advice, with regards to contact sports/ extremes of exercise such as rugby, kick boxing or body building, this should be discussed with your medical team.
The following exercises are taken from PhysioTools General Exercises, used with permission from PhysioTools LTD.
Exercise Programme
Sitting: Bend your head forward until you feel a stretch behind your neck. Hold approx 10 secs.
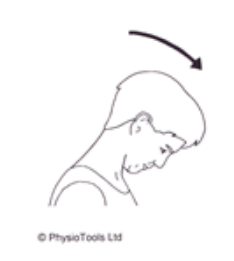
Sitting: Bend your head backwards as far as is comfortable. Hold approx 10 secs. Repeat 10 Times.
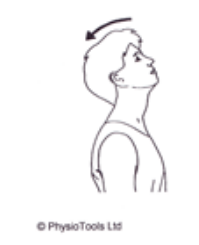
Sitting: Turn your head to one side until you feel a stretch. Hold approx. 10 secs. Repeat to other side. Repeat 10 times.
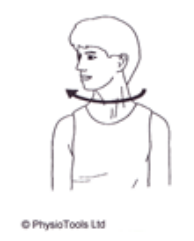
Sitting: Sitting straight-backed, push your head back against a firm surface. Pull your chin in, keeping your neck and back straight (not tipping your head forwards). Hold at the end position and feel the stretch in your neck.
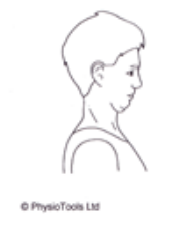
Sit or Stand. Roll your shoulders in both directions. Repeat 10 Times.
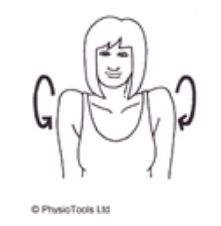
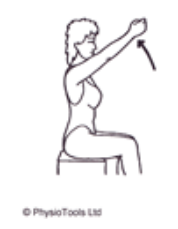
Sit or Stand. Lift both arms above head up letting the thumb lead the way. Repeat 10 Times.
If you have any queries, before or after your surgery please do not hesitate to contact us or speak to your GP.
Spinal Nurses 0151 556 3424
Physiotherapist 0151 556 3863
Secretary to your Consultant 0151 525 3611 and ask for your Consultant’s Secretary
- Last Updated:29 January 2024
- Review Date:29 January 2026
- Author:Keren Smallwood
- Summary:
The surgical procedure that you are to be admitted for is called a cervical disectonomy. This is performed for someone who has a prolapsed (slipped) disc in the neck area.