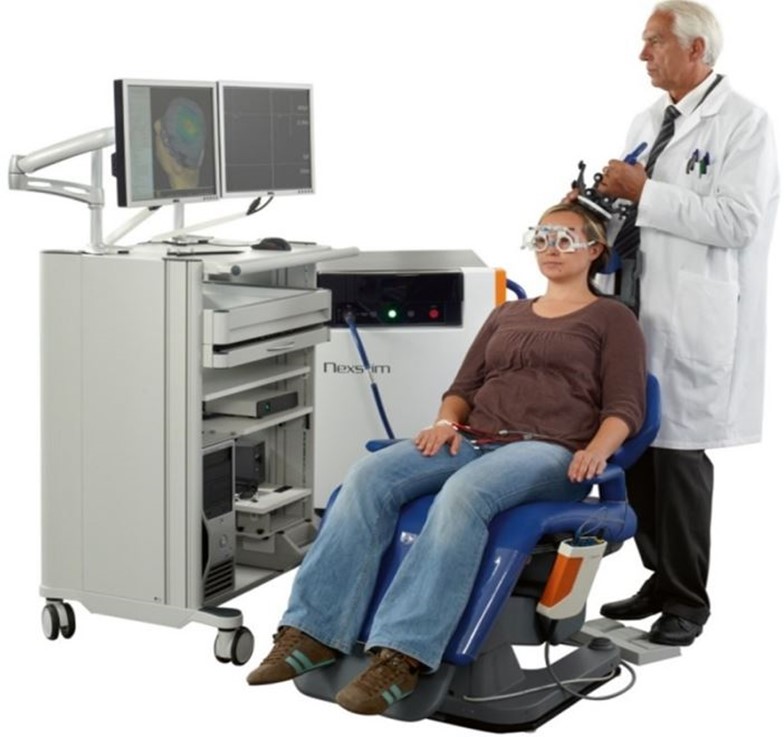
Transcranial magnetic stimulation (TMS) for chronic pain
What is chronic pain?
Pain messages are sent along special pain pathways and up the spinal cord to the brain. Although we may feel pain in a particular place, such as a joint, nerve or muscle, we only recognise the sensation as pain once it reaches the brain.
Acute pain occurs during and after harm or damage to part/s of the body. It is short-lived and fades away once healing has taken place. However, pain occasionally continues beyond the natural time of healing despite efforts to relieve it. If it has been present for six months or more, it is classified as chronic. Chronic pain is different from acute pain as it is felt in the absence of harm or damage, and therefore has no useful purpose. In the case of an acute pain it is helpful to rest the area to let it heal, but this natural response may be detrimental in the chronic pain leading to a vicious circle of pain and disability. Chronic pain can also give rise to other symptoms such as tiredness, boredom, depression or anxiety which can make the pain harder to cope with.
Although the exact cause of chronic pain is not known, there is good evidence to show that with it the nervous system undergoes many changes. Pain signals are spontaneously generated in the nerves which the brain interprets as real pain. It is as if a burglar alarm had gone off on its own without an intruder in the house. Many treatments are used to reduce these false alarm signals but they do not always work. Another curious change that happens is that the body’s ability to control pain is weakened when chronic pain sets in. Our ability to withstand pain, or distract from it, is reduced. In such a situation, a long distance runner who in a race can withstand enormous pain may find simple walking impossible because of a similar pain.
About transcranial magnetic stimulation (TMS)
It has been known for some time now that stimulation of the superficial layer of the brain, the cortex, can lead to a decrease of chronic pain. This is believed because on the one hand such stimulation interferes with inappropriate pain signals and on the other hand strengthens the way the brain combats the pain. In the latter case, the stimulation increases the signals that the brain sends down the spinal cord to interrupt abnormal pain signals. There are several types of brain stimulation that have been developed for this purpose, among them it’s the transcranial magnetic stimulation (TMS).
What exactly is TMS?
TMS is a non-invasive way to “switch on” very small parts of the brain by a series of magnetic pulses. To do that, we use an electromagnetic coil that sends pulses into the brain to generate a tiny electrical current. The brain then finds a way of using this current to stop pain signals. The changes that TMS induces in the brain are very small and mostly to do with the way brain cells communicate with each other. The effect is temporary because such changes are initially reversible. We do not know if they become established over time, but so far that has not been observed in any person receiving TMS.
To deliver TMS we use a plastic coated coil that is held against your head and sends the magnetic pulse through the skull into the brain. The exact positioning of the coil is determined by the location of your maximum pain. To pinpoint the target, we use an MRI scan of your head. As a rule of thumb, the optimal target on the cortex is the spot that controls the movement of a single muscle in the region of your pain. Once that has been established, the treatment consists of a series of pulses given over 10 or 20 seconds with a 30 second interval between them. This treatment will then be repeated as discussed below.
Each treatment is given while you are comfortably seated in a purpose-built chair. You will be totally awake and no sedation is needed.
How do you determine the precise brain location for TMS treatment?
This requires a separate ‘mapping session’ which we always do at the start. The critical aspect of the mapping is to make sure that the target muscle chosen by your doctor can be activated by TMS. We will place small (1 cm in diameter) recording electrodes on your hand, stuck on to the skin and are painless. We will then give several single pulses strong enough to cause a small movement (twitch) in your hand, leg, neck or head (depending on where your pain is), lasting a fraction of a second. The mapping session usually involves 20-25 pulses given every 5-15 seconds. We usually identify two separate targets, a ‘hotspot’ at which a TMS pulse gives the strongest response, and an alternative site where the response is slightly less. This information is saved on the system, so that at any subsequent session we will be able to identify it with no need for repeated mapping.
Can you use my previous MRI?
If you have had your MRI at the Walton Centre it usually can be used for our TMS. If you have had it taken a long time ago, it may have to be repeated because the human brain tends to change over time. If you had your previous MRI in another hospital, you are likely to need a new MRI that conforms to the specifics of the TMS computer programme we use.
Can I have a CT scan instead?
No, unfortunately not, because a CT scan will not provide the necessary details of the brain that we need.
How is TMS given and what will I feel?
You will be seated comfortably and your head will be resting on a padded support. You will wear a reflective sticker on your forehead. The TMS Operator will touch your scalp and ears using a small measuring rod. The computer is programmed to collate all information gathered this way and combine it with your MRI scan. The end result is that the movement of the coil in relation to your pain can be tracked in real time. The technique is similar to that used in SatNav devices.
With each pulse that is sent from the coil to your brain you will hear a clicking noise. During mapping, a single muscle twitch is produced. When TMS is given for treatment, no muscle twitching is produced. You will likely feel a strong tapping sensation on your scalp and may experience some jaw movement.
Approximately one-third report the scalp sensation as moderately painful. By contrast, it is likely that you feel nothing, or only a vague sensation, in the part of your body where you have your pain. One treatment session will last approximately 50 minutes, including the preparation time.
Do I need to prepare for a session in any way?
No preparation is needed. Before we offer you the first session you will have been assessed in the outpatient clinic and considered suitable for TMS by your pain consultant. There are a few reasons why some people should not have TMS. You must be over 16, not be pregnant, not have a cardiac pacemaker, not wear a cochlear implant, and not have any metallic implant, such as a brain or spinal cord stimulator in place. If you have ever suffered from fainting fits, we can only perform TMS if the information from your own doctor is that they have not been epileptic fits. If you have a history of drug or alcohol abuse, or if you have severe heart disease, we must check with your doctor that you are eligible. Some types of medications may affect the brain’s responses and we will assess each person carefully to make sure the TMS is safe.
Is TMS safe? What are the side effects?
TMS is generally considered safe but there are some safety issues you should know about. There are international guidelines that we follow carefully. The TMS coil causes a clicking noise which can sound quite loud if it is near the ear so you will be asked to wear earplugs. After a session, short-lived headache and fatigue are commonly reported but as a rule do not need treatment. Some subjects feel a little dizzy but are back to normal within 15 minutes. It is not uncommon for patients to report a temporary increase in their original pain which settles within days. The typical patient experience is that they feel normal and are allowed to leave the clinic immediately after the session.
We wish to point out, however, that some patients have experienced an epileptic seizure after TMS. Since the international guidelines have been in force, they have become very rare. A recent review reported only 2 cases of epileptic fits in thousands of sessions of TMS. We believe the risk of a single seizure exists but is very small. We minimise the risk by not offering TMS to people who have had a fit in the past or are using high doses of medication known to make fits more likely. The TMS Operator and other staff are trained in how to deal with a fit in the very unlikely event of one happening. It should be underlined that TMS does not cause epilepsy.
If you have an epileptic seizure triggered by TMS, you will need to notify the DVLA by law. You will also have to stop driving. There is no strict advice available about what happens next, and DVLA will deal with each case on an individual basis. We will also refer you to one of the epilepsy neurologists at the Walton Centre.
How long will any pain relief last?
When you have your first TMS session, the effect is likely to last only a day or two. With repeated sessions, the effect will get longer. However, some people will not benefit at all and this will become clear after 3-5 sessions. Those who do benefit will typically experience pain relief lasting 2-4 weeks, after which the treatment will have to be repeated to maintain the pain relief. Those who do not benefit will be reviewed by their pain consultant and most likely discharged back to the GP.
This means that even if you respond well to TMS, you only benefit from it long-term if you attend sessions on a regular basis. There is ongoing research, however, to establish whether a portable device delivering an electric current through the scalp is capable of achieving a similar effect. Such a device may be used at home on a daily basis and would make regular TMS sessions unnecessary. In rare cases neurosurgeons may be able to implant an electrode inside your head to lie over the brain to deliver an electric current. Best results are seen in those who respond well to TMS.
Please note that we cannot guarantee any ongoing treatment with TMS after the currently funded pilot period has elapsed and we might need to discharge the patient back to their GP.
Will I need to change my medication if I have TMS?
There are no strict rules, but we recommend reducing or tapering your current pain medication if it does not clearly help. Some medication may oppose the effect of TMS and is best avoided. Your specialist will be able to judge what is the best option for you. There is no need to change your other medication, e.g., that for high blood pressure, cholesterol or diabetes.
I am having other treatment for my pain which does not involve medication. Will it need to be modified?
No, there is no need to make any changes.
What is the current Walton Centre experience of TMS in the management of chronic pain?
Since 2011 we have provided TMS treatment for chronic pain, although only as part of research projects. All research has involved patients with chronic neuropathic pain who have not benefit from other treatments. We rate some 30% of patients as responders who show clinically meaningful improvement of their pain and are motivated to have long-term TMS treatment. We have treated around 200 people in over 3000 sessions. Some patients have received over 100 treatment sessions and continue to have a stable response and tolerate the treatment well. In some cases, people have complained of an increase in their existing tinnitus but specialist investigations have not shown a connection with TMS. We have seen one epileptic fit in one of our patients, which self-terminated and did not cause any problems except the inability to drive for 6 months.
Why am I being asked to keep a pain diary and fill in questionnaires?
We are at the moment the only NHS pain clinic in the country providing this service. Therefore, we are required to collect this information for auditing purposes. Your pain diaries help us to provide evidence of effectiveness that is used to compete for future NHS funding for this service. Other questionnaires deal with your overall response to the treatment, as well as safety and cost-effectiveness of the treatment which the funders must also have. Please note that all data are being treated confidentially and when sent forward will be anonymised.
Who can I contact if I have a question about TMS?
Your primary contact is the Walton Centre TMS Specialist Operator, Ms Anna Mavrianou, tel. 0151 529 5834/0151 556 3255, E-mail address anna.mavrianou@nhs.net. The office hours in general are Monday to Friday 10.00 – 16.30. She will be able to deal with your query or contact your Pain Consultants if required. At the moment we do not provide an out of hours service.
The Walton Centre NHS Foundation Trust
Lower Lane
Fazakerley
Liverpool
L97LJ
Tel: 0151 525 3611
- Last Updated:01 May 2023
- Review Date:01 May 2026
- Author:Dr B Frank
- Summary:
Transcranial magnetic stimulation for chronic pain